
We use cookies to ensure our website works properly and to personalise your experience. Cookies policy

We use cookies to ensure our website works properly and to personalise your experience. Cookies policy
1,5,6,7 Department of Family Medicine, Tabuk Health Cluster, Tabuk, SAU
2,3,4 Academic Affairs, Family Medicine Residency Training Program, Tabuk Health Cluster, Tabuk, SAU
Stress and burnout are increasingly recognized as significant issues affecting resident physicians, impacting their performance, mental health, and patient care. This study aimed to assess the prevalence and contributing factors of stress and burnout among family medicine residents in Tabuk City, Saudi Arabia. A cross-sectional study was conducted between December 2023 and June 2024 among 100 family medicine residents from the Ministry of Health and King Khalid Military Hospital programs in Tabuk. A self-administered online questionnaire, distributed via social media platforms, was used to collect data on sociodemographic variables, work-related characteristics, and stressors. Stress was assessed using 24 validated binary (Yes/No) items across five domains. Stress levels were categorized as low (0–8), moderate (9–16), or high (17–24). Data were analyzed using SPSS version 28, and chi-square or exact probability tests were used to explore associations. Among the 100 residents, 47.0% reported moderate stress levels, 30.0% low, and 23.0% high. Common stressors included fear of making mistakes (77.0%), time pressure (76.0%), and work-life imbalance (73.0%). Statistically significant factors associated with higher stress included being single (p = 0.027), having a distinction-level academic record (p = 0.049), longer duration of residency (p = 0.048), high-stress rotations such as Obstetrics & Gynecology (p = 0.001), working ?72 hours per week (p = 0.035), and smoking (p = 0.001). A considerable proportion of family medicine residents in Tabuk experience moderate to high levels of stress and burnout, influenced by both personal and systemic factors. Targeted interventions, such as workload regulation, improved mentorship, and psychological support, are recommended to enhance resident well-being and program sustainability.
Burnout is a psychological condition that arises from prolonged occupational stress combined with the depletion of an individual’s ability to cope effectively [1]. It is commonly assessed through three key dimensions: emotional exhaustion, depersonalization, and reduced personal accomplishment [2]. These dimensions are typically measured using the Maslach Burnout Inventory (MBI), a widely validated tool in medical and occupational research [3].
Burnout among medical residents remains a critical global health issue, with studies reporting prevalence rates ranging from 40-82% across different regions and specialties [4, 5]. International data shows particularly high rates in surgical (60-82%) and emergency medicine (55-75%) residents [6, 7], while family medicine trainees typically experience slightly lower but still significant rates (45-70%) [8, 9]. In the Middle East, prevalence appears even higher, with Saudi studies reporting 84.2% burnout among family medicine residents [10], significantly exceeding global averages. These elevated regional rates may reflect extended work hours, high patient loads, and unique training challenges.
Burnout scores revealed limited significant associations with some variables; however, noteworthy relationships emerged between burnout levels and factors such as remorse-related personality traits, environmental conditions, and background characteristics [11, 12]. These findings underline the critical role of personal comfort and interpersonal skills in mitigating burnout. Reviewing the current experience of stress and burnout across family medicine residents in Tabuk City family medicine programs is the goal of this study.
METHODOLOGY
This study applied a cross-sectional design targeting family medicine residents enrolled in residency programs in Tabuk City, Saudi Arabia. The study area includes family medicine residency programs affiliated with the Ministry of Health and King Khalid Military Hospital in Tabuk, a city located along the north-west coast of Saudi Arabia with a population of approximately 657,000. The data collection period reaches over six months, from December 1, 2023, to June 30, 2024. The study population consisted of all family medicine residents (both male and female) training in Tabuk during 2024, including residents in their first, second, and third years. A total population of 100 residents was targeted, with a confidence interval of 95% and a margin of error of 5%. Residents from other specialties or with chronic diseases such as diabetes, hypertension, asthma, or diagnosed psychiatric disorders were excluded from the study to reduce confounding factors.
Data were collected using a self-administered online questionnaire distributed through social media platforms to all eligible residents. Before the full study, a pilot test was conducted to assess the validity and reliability of the questionnaire. The internal consistency of the instrument was evaluated using Cronbach’s alpha, which yielded a value of 0.72, indicating acceptable reliability. The questionnaire consisted of three parts. The first part gathered sociodemographic and work-related characteristics, including age, gender, marital status, smoking and alcohol habits, university of graduation, graduate qualifications, duration of residency training, current rotation, and weekly working hours. The second part assessed sources of job stress using validated items adapted from previously published studies. Residents were asked to indicate whether specific stressors, such as “fear of making mistakes,” “work overload and on-call duties,” “worries about finances,” and “feeling insecure in this job,” caused them stress, with responses recorded as “Yes” or “No.” This tool allowed for a comprehensive evaluation of stress and burnout factors among the study population.
DATA ANALYSIS
Data were analyzed using SPSS version 28 (IBM Corp., Armonk, NY, USA). Descriptive statistics were computed for sociodemographic variables, residency characteristics, and stress-related factors. Stress and burnout levels were assessed using a binary scoring system (0 = absence, 1 = presence) for each stressor item. The total stress score was calculated by summing individual stressor scores, resulting in a possible range from 0 to 24. For categorization, the overall stress/burnout level was divided into three simplified levels based on the total score: Low Stress (0–8): Few stressors present; indicative of manageable stress. Moderate Stress (9–16): Several stressors present; may affect performance or well-being. High Stress (17–24): Many stressors present; reflects a high risk of burnout or job dissatisfaction. Inferential statistics included chi-square tests to evaluate associations between stress/burnout levels and categorical demographic and work-related variables. Where cell counts were low, exact probability tests were applied. Statistical significance was set at a p-value of less than 0.05.
RESULTS
Table 1. Sociodemographic Characteristics of Family Medicine Residents in Tabuk City, Saudi Arabia (2023) (N=100)
|
Data |
No |
% |
|
Age in years |
||
|
25-27 years |
41 |
41.0% |
|
> 27 years |
59 |
59.0% |
|
Gender |
||
|
Male |
33 |
33.0% |
|
Female |
67 |
67.0% |
|
Marital status |
||
|
Single |
60 |
60.0% |
|
Married |
40 |
40.0% |
|
University of graduation |
||
|
International |
9 |
9.0% |
|
Local private |
4 |
4.0% |
|
Local public |
87 |
87.0% |
|
Graduate qualification |
||
|
Distinction |
2 |
2.0% |
|
Honor |
36 |
36.0% |
|
Pass |
62 |
62.0% |
Table 1 presents the sociodemographic characteristics of the family medicine residents participating in the study. Of the total 100 residents, 41 (41.0%) aged between 25 and 27 years, while the majority, 59 (59.0%), were older than 27 years. Regarding gender distribution, 33 residents (33.0%) were male and 67 (67.0%) were female. Regarding marital status, 60 residents (60.0%) were single, whereas 40 (40.0%) were married. The majority of the residents graduated from local public universities, representing 87 (87.0%) of the sample, while only 9 (9.0%) graduated from international universities and 4 (4.0%) from local private universities. Concerning graduate qualification, 62 residents (62.0%) passed, 36 (36.0%) achieved honors, and 2 (2.0%) graduated with distinction.
Table 2. Residency and Lifestyle of Family Medicine Residents in Tabuk City, Saudi Arabia (2023) (N=100)
|
Residency data |
No |
% |
|
Duration in residency training |
||
|
≤12 months |
34 |
34.0% |
|
13–24 months |
22 |
22.0% |
|
>24 months |
44 |
44.0% |
|
Current rotation |
||
|
Family medicine |
40 |
40.0% |
|
Emergency Medicine |
12 |
12.0% |
|
Pediatrics |
12 |
12.0% |
|
Medicine |
10 |
10.0% |
|
Orthopedics |
8 |
8.0% |
|
Dermatology |
4 |
4.0% |
|
Obstetrics & Gynecology |
4 |
4.0% |
|
Board certified |
2 |
2.0% |
|
Pediatric ER |
2 |
2.0% |
|
Psychiatry |
2 |
2.0% |
|
Radiology |
2 |
2.0% |
|
Surgery |
2 |
2.0% |
|
Work hours/week |
||
|
< 40 hours |
26 |
26.0% |
|
60 hours |
55 |
55.0% |
|
72 hours |
19 |
19.0% |
|
Smoking |
||
|
Yes |
4 |
4.0% |
|
No |
96 |
96.0% |
|
Alcohol |
||
|
Yes |
0 |
0.0% |
|
No |
100 |
100.0% |
Table 2 summarizes the residency data among family medicine residents. Regarding residency duration, 34 residents (34.0%) had been in training for 12 months or less, 22 (22.0%) for 13 to 24 months, and the largest group, 44 residents (44.0%), had been in training for more than 24 months. The current rotation differs, with the highest proportion being 40 residents (40.0%) in family medicine, followed by 12 residents (12.0%) in emergency medicine and pediatrics. Other rotations had smaller representation, including medicine (10.0%), orthopedics (8.0%), dermatology and obstetrics & gynecology (4.0% each), and several other specialties at 2.0% each. The majority of residents (55.0%, n=55) worked 60 hours per week, while 26 residents (26.0%) worked less than 40 hours, and 19 residents (19.0%) worked 72 hours per week. Concerning lifestyle factors, only 4 residents (4.0%) reported smoking, and none reported alcohol consumption.
Table 3. Prevalence of Stressors Among Family Medicine Residents by Stress Domain in Tabuk City, Saudi Arabia (2023) (N=100)
|
Domain |
Stressor |
Yes |
No |
||
|
No |
% |
No |
% |
||
|
Clinical Practice Stressors |
Fear of making mistakes |
77 |
77.0% |
23 |
23.0% |
|
Time pressures and difficulty meeting deadlines |
76 |
76.0% |
24 |
24.0% |
|
|
Working with uncooperative and incompetent colleagues |
46 |
46.0% |
54 |
54.0% |
|
|
Work overload and on-call duties |
40 |
40.0% |
60 |
60.0% |
|
|
Work demands affect personal and home life |
73 |
73.0% |
27 |
27.0% |
|
|
Inadequate skills for dealing with difficult aspects of work |
49 |
49.0% |
51 |
51.0% |
|
|
The feeling of inadequate knowledge and skills to meet work demands |
55 |
55.0% |
45 |
45.0% |
|
|
Workplace Environment Stressors |
Lack of adequate, comfortable restrooms and facilities |
76 |
76.0% |
24 |
24.0% |
|
Lack of incentives and promotions |
59 |
59.0% |
41 |
41.0% |
|
|
Feeling of underpaid |
45 |
45.0% |
55 |
55.0% |
|
|
Lack of resources |
46 |
46.0% |
54 |
54.0% |
|
|
Feeling unsafe during work |
31 |
31.0% |
69 |
69.0% |
|
|
Feeling insecure in this job |
37 |
37.0% |
63 |
63.0% |
|
|
Interpersonal & Supervisory Stressors |
Lack of support and unfair assessment from the supervisor |
54 |
54.0% |
46 |
46.0% |
|
Difficulty maintaining relationships with supervisors |
44 |
44.0% |
56 |
56.0% |
|
|
Working outside one’s competence |
41 |
41.0% |
59 |
59.0% |
|
|
Psychological & Emotional Stressors |
Fear of infection |
66 |
66.0% |
34 |
34.0% |
|
Worries about finances |
42 |
42.0% |
58 |
58.0% |
|
|
Feeling insecure in this job |
41 |
41.0% |
59 |
59.0% |
|
|
Fear of making mistakes |
73 |
73.0% |
27 |
27.0% |
|
|
Workload & Career Progression Stressors |
Work overload |
68 |
68.0% |
32 |
32.0% |
|
On-call duties |
41 |
41.0% |
59 |
59.0% |
|
|
Career-related worries (insecurity, financial instability) |
50 |
50.0% |
50 |
50.0% |
|
Table 3 illustrates the stressors among family medicine residents across different domains. Within the Clinical Practice Stressors, the most frequently reported stressors were fear of making mistakes (77.0%), time pressures and difficulty meeting deadlines (76.0%), and work demands affecting personal and home life (73.0%). For Workplace Environment Stressors, residents most commonly reported lack of adequate, comfortable restrooms and facilities (76.0%), lack of incentives and promotions (59.0%), and feeling underpaid (45.0%). In the Interpersonal & Supervisory Stressors domain, the leading stressors were lack of support and unfair assessment from supervisors (54.0%), difficulty maintaining relationships with supervisors (44.0%), and working outside one’s competence (41.0%). Under Psychological & Emotional Stressors, residents predominantly experienced fear of making mistakes (73.0%), fear of infection (66.0%), and worries about finances (42.0%). Finally, in the Workload & Career Progression Stressors, the most reported stressors included work overload (68.0%), career-related worries such as insecurity and financial instability (50.0%), and on-call duties (41.0%).
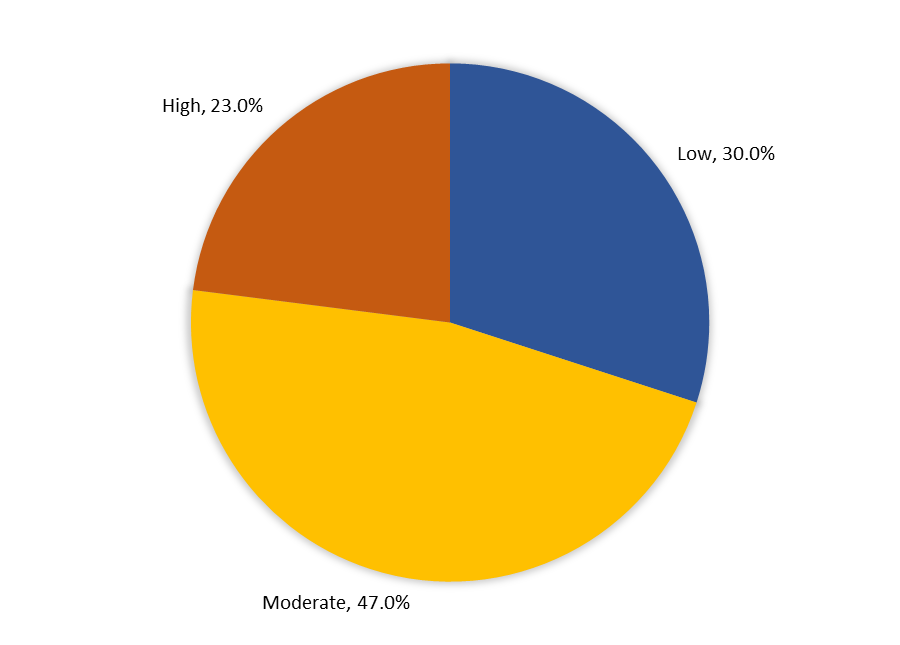
Figure 1. The Overall Stress / Burnout Level Among Family Medicine Residents in Tabuk City, Saudi Arabia (2023) (N=100)
Figure 1 shows the overall stress and burnout levels among family medicine residents in Tabuk City. Nearly half of the residents, 47 (47.0%), experienced a moderate level of stress or burnout. About 30 residents (30.0%) reported a low level, meanwhile 23 residents (23.0%) experienced a high level of stress or burnout.
Table 4. Factors Associated with Stress / Burnout Among Family Medicine Residents in Tabuk City
|
Factors |
Overall stress/burnout level |
p-value |
|||||
|
Low |
Moderate |
High |
|||||
|
No |
% |
No |
% |
No |
% |
||
|
Age in years |
.239 |
||||||
|
25-27 years |
16 |
39.0% |
16 |
39.0% |
9 |
22.0% |
|
|
> 27 years |
14 |
23.7% |
31 |
52.5% |
14 |
23.7% |
|
|
Gender |
.673 |
||||||
|
Male |
8 |
24.2% |
17 |
51.5% |
8 |
24.2% |
|
|
Female |
22 |
32.8% |
30 |
44.8% |
15 |
22.4% |
|
|
Marital status |
.027* |
||||||
|
Single |
14 |
23.3% |
27 |
45.0% |
19 |
31.7% |
|
|
Married |
16 |
40.0% |
20 |
50.0% |
4 |
10.0% |
|
|
University of graduation |
.060^ |
||||||
|
International |
6 |
66.7% |
3 |
33.3% |
0 |
0.0% |
|
|
Local private |
2 |
50.0% |
2 |
50.0% |
0 |
0.0% |
|
|
Local public |
22 |
25.3% |
42 |
48.3% |
23 |
26.4% |
|
|
Graduate qualification |
.049*^ |
||||||
|
Distinction |
0 |
0.0% |
0 |
0.0% |
2 |
100.0% |
|
|
Honor |
10 |
27.8% |
15 |
41.7% |
11 |
30.6% |
|
|
Pass |
20 |
32.3% |
32 |
51.6% |
10 |
16.1% |
|
|
Duration in residency training |
.048* |
||||||
|
≤12 months |
16 |
47.1% |
12 |
35.3% |
6 |
17.6% |
|
|
13–24 months |
2 |
9.1% |
14 |
63.6% |
6 |
27.3% |
|
|
>24 months |
12 |
27.3% |
21 |
47.7% |
11 |
25.0% |
|
|
Current rotation |
.001*^ |
||||||
|
Board certified |
0 |
0.0% |
2 |
100.0% |
0 |
0.0% |
|
|
Dermatology |
4 |
100.0% |
0 |
0.0% |
0 |
0.0% |
|
|
Emergency Medicine |
2 |
16.7% |
6 |
50.0% |
4 |
33.3% |
|
|
Family medicine |
12 |
30.0% |
21 |
52.5% |
7 |
17.5% |
|
|
Medicine |
6 |
60.0% |
2 |
20.0% |
2 |
20.0% |
|
|
Obstetrics & Gynecology |
0 |
0.0% |
0 |
0.0% |
4 |
100.0% |
|
|
Orthopedics |
4 |
50.0% |
4 |
50.0% |
0 |
0.0% |
|
|
Pediatric ER |
0 |
0.0% |
2 |
100.0% |
0 |
0.0% |
|
|
Pediatrics |
0 |
0.0% |
6 |
50.0% |
6 |
50.0% |
|
|
Psychiatry |
0 |
0.0% |
2 |
100.0% |
0 |
0.0% |
|
|
Radiology |
0 |
0.0% |
2 |
100.0% |
0 |
0.0% |
|
|
Surgery |
2 |
100.0% |
0 |
0.0% |
0 |
0.0% |
|
|
Work hours/week |
.035* |
||||||
|
< 40 hours |
12 |
46.2% |
12 |
46.2% |
2 |
7.7% |
|
|
60 hours |
16 |
29.1% |
26 |
47.3% |
13 |
23.6% |
|
|
72 hours |
2 |
10.5% |
9 |
47.4% |
8 |
42.1% |
|
|
Smoking |
.001*^ |
||||||
|
Yes |
0 |
0.0% |
0 |
0.0% |
4 |
100.0% |
|
|
No |
30 |
31.3% |
47 |
49.0% |
19 |
19.8% |
|
P: Pearson X2 test ^: Exact probability test * P < 0.05 (significant)
Table 4 outlines the factors associated with stress and burnout levels among family medicine residents. Marital status was significant (p = 0.027), with a higher proportion of single residents (31.7%) experiencing high stress compared to married residents (10.0%). Graduate qualification also showed a significant association (p = 0.049), where all residents with distinction were in the high stress group. Duration of residency training was linked to stress levels (p = 0.048); residents with ≤12 months of training were more likely to report low stress (47.1%), while those with longer training durations had higher moderate and high stress levels. The current rotation had a strong impact on stress (p = 0.001), notably with 100% of residents in Obstetrics & Gynecology reporting high stress, while rotations such as Dermatology and Surgery had residents predominantly in the low stress group. Work hours per week were also significant (p = 0.035), as those working 72 hours weekly had the highest proportion of high stress (42.1%) compared to just 7.7% in residents working less than 40 hours. Smoking status was strongly associated with stress (p = 0.001); all smokers (100%) reported high stress, while none were in the low or moderate groups. Other factors like age and gender did not show significant associations with stress or burnout levels.
DISCUSSION
The study on burnout and anxiety among family medicine residents in Tabuk City, Saudi Arabia (2023), included 100 participants with different sociodemographic characteristics. The majority of residents were over 27 years old, with a higher proportion of females than males. Most participants were single, and a significant number had graduated from local public universities. Considering academic achievement, most residents had passed their qualifications, while a smaller proportion graduated with honors or distinction.
The findings on residency-related factors reveal some variations in training duration, current rotations, workload, and lifestyle habits among family medicine residents in Tabuk City. A substantial proportion of residents had been in training for over 24 months, indicating that long-term exposure to residency demands may influence burnout and stress levels. The distribution across rotations varied, with family medicine being the most common, followed by emergency medicine and pediatrics, which may reflect differing stressors based on specialty-specific demands. Workload patterns also differed, with a majority working extended weekly hours, a known risk factor for burnout. Interestingly, smoking was rare, and alcohol consumption was absent, matching with cultural norms in Saudi Arabia.
The study identifies key stressors among family medicine residents in Tabuk City that align with global and regional findings. High rates of fear of making mistakes and time pressures reflect common anxieties in medical training, consistent with previous research highlighting workload and patient safety concerns [13, 14]. Work demands affecting personal life further confirm links to emotional exhaustion in demanding medical environments [15]. Systemic issues such as inadequate facilities, underpayment, and lack of incentives mirror challenges reported in Middle Eastern residency programs, emphasizing the need for institutional reforms [16, 17]. Interpersonal stressors, including poor supervisory support and difficult relationships, resonate with findings that hierarchical, unsupportive supervision increases burnout risk [18, 19]. Psychological stressors like fear of infection and financial worries echo global post-pandemic concerns and economic strains among trainees [20, 21]. Lastly, workload pressures, career insecurity, and on-call duties match with established burnout factors tied to job instability and sleep deprivation [22, 23]. Together, these results highlight complex stress sources requiring comprehensive strategies to improve resident well-being [24].
Generally, our study reveals that about half of family medicine residents experienced moderate stress/burnout, while one-fourth reported high levels, consistent with global trends but showing some regional variations. Comparable studies demonstrate wide-ranging burnout prevalence among medical residents, from 18% to 82% [25], meaning that institutional and cultural factors significantly influence these rates. The 30% low-stress group in Tabuk contrasts with findings from Aseer, Saudi Arabia (84.2% burnout prevalence) [17] and British Columbia (70% burnout) [26], possibly due to differences in workload, support systems, or measurement tools. However, the high-stress level (23%) simulates reports from Ontario, where residents experienced elevated anxiety (12%) and depression [16], reinforcing that medical training universally poses psychological risks.
Notably, studies in South Carolina [27] and East Tennessee [28] found lower stress levels, attributing this to strong social support and stress-management programs, factors that may be underdeveloped in Tabuk. The moderate-stress majority suggests partial resilience, possibly due to protective factors like mentorship and work appreciation, but also highlights unmet needs in workload management and emotional support.
As for factors associated with stress/burnout, single residents experienced significantly higher stress compared to married peers, supporting literature on the protective role of marital support [29], though differing from Alghamdi’s Saudi findings that linked marriage to greater emotional exhaustion [26]. High stress among residents with distinction-level academic achievement is in line with research identifying perfectionism as a burnout risk factor [25], suggesting high achievers may face greater internal pressure. Longer residency duration was associated with increasing stress, supporting evidence that burnout accumulates over time during training [30, 31]. A strong association between smoking and high stress raises concern, potentially reflecting stress-driven smoking behaviors or reduced coping capacity in smokers.
CONCLUSION
This study revealed that stress and burnout are highly prevalent among family medicine residents in Tabuk City, with nearly half experiencing moderate levels and almost a quarter facing high levels of stress. The most common stressors were clinical, such as fear of making mistakes and time pressure, as well as environmental issues like inadequate facilities and lack of incentives. Psychological stress and concerns about career progression also played a major role in residents’ well-being. Certain groups were particularly vulnerable: single residents, those with high academic achievement, residents working long hours, and those in certain high-demand rotations such as Obstetrics & Gynecology. It is recommended that residency programs implement structured mental health support, promote a more supportive supervisory environment, and consider rotation and workload balancing. Additionally, improvements in infrastructure, transparent promotion pathways, and targeted interventions for high-risk groups, such as new residents or those working excessive hours, could reduce stress and enhance overall resident well-being.
REFERENCES







Arub Mohammed Albalawi, Marwa Gamal Mohammed, Ahmed Raja Albalawi, Asma Ali Alharbi, Wejdan Mohammed Alshehri, Wejdan A. Alshehri, Nagham Mohammad Alkhrissi, Knowledge, Attitude, And Practice Towards Burnout and Anxiety Among Family Medicine Residents in Family Medicine Programs in Tabuk City, Saudi Arabia, 2023, Cross-Sectional Study, Int. J. of Pharm. Sci., 2025, Vol 3, Issue 8, 1583-1593. https://doi.org/10.5281/zenodo.16875472
 10.5281/zenodo.16875472
10.5281/zenodo.16875472