Abstract
The U.S. Agency for International Development is assisting in the creation and execution of a national strategy to strengthen local coalitions, advocacy, and activity packages in order to address the escalating issue of antimicrobial resistance (AMR). In Zambia, this strategy is being piloted. A meeting with several stakeholders was held in Lusaka by the local AMR Advocacy Working Group (AWG), which was established to assist with the process. Seventy stakeholders representing the government, academia, service providers (nurses, pharmacists, and medical and veterinary doctors), professional associations, consumers, journalists, industry, the private sector, and cooperating partners attended the meeting, which was opened by the honourable Minister for Health of the Government of the Republic of Zambia. The findings, actions, and suggestions of a group of partners that travelled to Zambia to support the AWG are detailed in this report. The primary thrust of this activity is to catalyse an initial response by local stakeholders to build and scale up coalition, commonalities, and advocacy. Pilot testing of the approach is underway in Zambia. An exploratory visit to Zambia revealed significant interest and concern over the issue of AMR and many stakeholders were willing to contribute to advocacy and AMR containment efforts. Two subsequent visits to initiate the process.
Keywords
Respiratory Tract Infections, Antibiotic Resistance, Knowledge, Attitude, Practice.
Introduction
A respiratory tract infection (RTI) is an infection that affects the respiratory system, which is the part of the body that allows you to breathe[I]. RTIs can affect the throat, sinuses, airways, or lungs. Upper respiratory tract infections (URTIs) include the common cold, laryngitis, pharyngitis/tonsillitis, acute rhinitis, acute rhinosinusitis and acute otitis media. Lower respiratory tract infections (LRTIs) include acute bronchitis, bronchiolitis, pneumonia and tracheitis [2]. Antibiotics are commonly prescribed for RTIs in adults and children in primary care. One of the main risks to world health is antibiotic resistance. We evaluated community pharmacists' actions, attitudes, and knowledge regarding antimicrobial stewardship and antibiotic resistance[3] . Using a standardized questionnaire, we performed a descriptive cross-sectional study with 144 community pharmacists who were chosen at random. Version 22 of the Statistical Package for Social Sciences was used to analyze the data at a 95% confidence level[4]. A 91% response rate (n=144) was attained [4]. Male community pharmacists between the ages of 30 and 39 made up the majority (63%) of the workforce. Remarkably, 67% had positive attitudes and 93.8% had strong knowledge[5]. On the other hand, 75% of community pharmacists showed inadequate antimicrobial stewardship and antibiotic resistance measures. despite the fact that community pharmacists were knowledgeable and had nice dispositions. Promoting antimicrobial stewardship is necessary.
METHODS
Study Design and Site
From March to August 2019, a descriptive cross-sectional study was carried out in Lusaka, Zambia, at community pharmacies. More than half of Zambia's registered community pharmacies are located in Lusaka, the country's capital. Registered CPs who gave their agreement to engage in the study were involved. This survey excludes drug stores, unregistered pharmacies, pharmacy technologists, and dispensers.
Sample size
Slovin's formula was used to determine the sample size. The sample size was calculated using a 5% margin of error and a 95% confidence level. The Zambia Medicines Regulatory Authority (ZAMRA) Register, which listed 225 registered community pharmacies in Lusaka at the time of the study, was used to choose the community pharmacists using simple random sampling.
Data collection tool: Structure self-administered questionnaire
A standardized, self-administered questionnaire was used to collect data. Similar research were used to adopt and modify the questionnaire. Pharmacy specialists pre-validated the questionnaire for accuracy, simplicity, clarity, understandability, and relevance. This allowed the original questionnaire to be modified. Twelve community pharmacists later pretested the questionnaire to ensure it was consistent. Data on the sociodemographic traits, knowledge, attitudes, and practices of community pharmacists regarding antibiotic resistance and AMS were then gathered using the final constructed questionnaire.
Data analysis
Version 22.0 of the Statistical Package for the Social Sciences (SPSS) was used to analyze the data. Before being exported to SPSS, data was first entered into a Microsoft Excel spreadsheet. A Likert scale was employed to assess the degree of knowledge, attitude, and practices, and the data was displayed as tables and figures. At a 95% confidence level, statistical significance was defined as p<0>
Ethical approval
The study was approved by the University of Zambia Health Sciences Research Ethics Committee (UNZAHSREC), protocol ID: 20190217024, IORG no: 0009227, IRB no: 00011000. All participants provided consent by reading and signing the consent form prior to responding to the questionnaire.
RESULTS
Demographic characteristics of participants
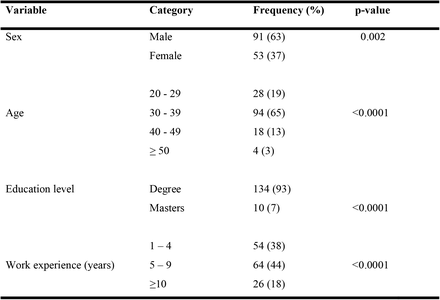
The demographic characteristics of 144 community pharmacists (CPs) who took part in the study are shown in Table 1. Most of the respondents were male (63%) and were aged between 30 and 45 years (65%).
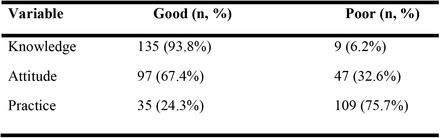
Overall knowledge, attitude, and practice scores on antibiotic resistance and AMS
The majority of the CPs 93.8% (n=135) had good knowledge and 67.4% had positive attitude with regards to antibiotic resistance. Unfortunately, 75.7% of the CPs had poor practice regarding antibiotic resistance and antimicrobial stewardship(Table 2)

Relationships between sociodemographic characteristics and knowledge, attitude, and practices
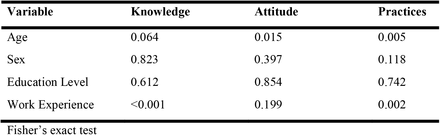
Statistical significance was found between age and attitude, age and practices, work experience and knowledge, and work experience and practices (Table 3)
DISCUSSION
We assessed that knowledge, attitude, and practice of community pharmacists (CPs) on antibiotic resistance and antimicrobial stewardship. Currently, there is limited information about the knowledge, attitude, and practice of CPs on antibiotic resistance and AMS in Zambia.
Community pharmacists’ knowledge of antibiotic resistance
Our study found that 93.8% of CPs had good knowledge of antibiotic resistance that was related to their work experience. In our study, the majority of the CPs strongly agreed that antibiotic resistance occurs when antibiotics fail to treat bacterial infections and that it usually occurs when there is overuse and misuse of antibiotics.
Attitudes of community pharmacists towards antibiotic resistance
Our study found that 67.4% of the CPs had a positive attitude towards antibiotic resistance that was related to their age. Our findings are encouraging because the positive attitude of CPs may influence them not to dispense antibiotics without a prescription. The majority of the community pharmacists in our study agreed that the appropriate use of antibiotics can reduce problems of antibiotic resistance.
Practices community pharmacists towards antibiotic resistance and AMS
Our study revealed that the majority (75.7%) of CPs had a poor practice regarding antibiotic resistance and AMS. The younger and less experienced CPs showed poorer practices compared to the older and experienced CPs. In Pakistan, similar results were reported. Poor practice towards antibiotic resistance calls for quick educational intervention programmes among CPs . Their practice could be affected by lack of continuing education and other external factors. Our study highlighted that the majority (68.8%) of the CPs often dispensed antibiotics on prescriptions with complete clinical information.
Limitation Of The Study
We acknowledge that the current study has some limitations. It focused on assessing the knowledge, attitude, and practices of community pharmacist leaving out pharmacy technologists who work under the supervision of the pharmacists. Therefore, the results should be interpreted in the context of community pharmacists. The study only focussed on registered community pharmacists and this could create a bias on the findings as illegal drug outlets are a nuisance in the country and could be the important drivers of antibiotic resistance and hamper the efforts towards AMS activities.
CONCLUSON
Community pharmacists in Lusaka Zambia had good knowledge and attitude but poor practices regarding antibiotic resistance. There is a need to promote ASPs in community pharmacies that may lead to the improved practice of community pharmacists with regards to antibiotic use, resistance, and AMS. Community pharmacists must be recognized as key players in the control and prevention of infections among community members. Therefore, educational intervention programmes with regards to antibiotic use, resistance, and AMS should be periodically focussed on community pharmacy practice.
REFERENCES
-
-
-
- Gautret, P.; Benkouiten, S.; Al-Tawfiq, J.A.; Memish, Z.A. Hajj-associated viral respiratory infections: A systematic review. Travel Med. Infect. Dis. 2016, 14, 92–109.
- Al-Tawfiq, J.A.; Zumla, A.; Memish, Z.A. Respiratory tract infections during the annual Hajj: Potential risks and mitigation strategies. Curr. Opin. Pulm. Med. 2013, 19, 192–197.
- Puriatarza, E.; Kamso, S. Cause of Death of Indonesia Hajj in Armenia, Saudi Arabia 2015. KnE Life Sci. 2018, 2019, 115–122
- Zuraina, N.M.N.; Sarimah, A.; Suharni, M.; Hasan, H.; Suraiya, S. High frequency of Haemophilus influenzae associated with respiratory tract infections among Malaysian Hajj pilgrims. J. Infect. Public Health 2018, 11, 878–883.





 10.5281/zenodo.14836351
10.5281/zenodo.14836351