
We use cookies to ensure our website works properly and to personalise your experience. Cookies policy

We use cookies to ensure our website works properly and to personalise your experience. Cookies policy
RMES’s college of Pharmacy, Kalaburagi
Background: To conduct a prospective observational study on prescribing pattern, follow-up pattern and impact of pharmacist initiated educational intervention on medication adherence in patient with psychiatric disorder. Aim And Objectives: The aim of this study is to evaluate the impact of clinical pharmacist interventions in the psychiatric setting in patient with psychiatric disorders. To find out the prescription pattern and follow up pattern of anti-psychotic medication in department of psychiatry. To identify the drug related problems of anti-psychotic medication in psychiatric patients. To improve the medication adherence of psychiatric patients. Methods: A Prospective interventional study of 6 months was conducted. Undertaken 102 patients’ data collection form of all the patient of outpatient department of age 18 ? years of psychiatric disorder with or without co-morbidity. Results: The results of this analysis suggest that out of the total 102 psychiatric patient included in the study 59 patient were males while 43 patients were females. Out of the total study subject, among the 102 psychiatric patients, patient with psychosis were found to be 40(39.21%), followed by insomnia 14(13.72%), schizophrenia 13(12.74%), anxiety disorder 12(11.76%), bipolar disorder 7(6.86%), anger disorder 5(4.90%), depression 5(4.90%), and with other psychiatric disorder were 6(5.88%). Conclusion: This study concludes that psychiatric disorder was more seen in male patient compared to female patients most of them were in the age of 31-45 years constituting of 37.25% of total patients during the study it is observed that Risperidone was the most commonly prescribed Anti-psychotic drug and it was mostly prescribed with Trihexyphenidyl.
Psychiatry disorders also known as mental health disorders or psychiatric illnesses these are conditions that affect a person's thoughts, feelings, behaviors, and overall well-being.1It is found that the majority of mental disorders arise from low and middle-income families 2Mental health disorders imitate a leading public health concern and cause high levels of disability and generally unrecognized and untreated as well and often possess several challenges in carrying out daily activities3. Almost 1 in 5 adults experiences mental illness and distress in 2019 year according to National Alliance of Mental Illness (NAMI)3. Out of top 10 health condition contributing to disability adjusted life years (DALY ‘s) 4 are psychiatric disorders.4. It is estimated that around 14.3% of all deaths globally can be attributed to mental disorders each year. The WHO has developed several different resources and initiatives aimed at addressing the public health issue of mental health5. At some point in time in life, behavioral and mental disorders commence in 10% of the adult population, and it contributes more than 12% of global disease burden6.In this population stigma has been a significant obstacle to the provision of effective care for people with mental illness7. The World Health Organization (WHO) has advised pharmacists to play an active role within multidisciplinary teams (MDTs) to improve psychotropic drug use in Psychiatric Disorders which are characterized by a clinically significant disturbance in an individual’s cognition, emotional regulation, or behavior8. The aim of the study is to determine prescription pattern, follow-up pattern and psychotropic medication adherence in a tertiary care teaching hospital Gulbarga institute of medical science (GIMS) gulbarga9.
METHODOLOGY
Study Duration: The study was conducted for a period of Six month: March - August 2024.
Study Design: This study is prospective intervention study.
Study Site: Study was conducted in outpatient setup of department of psychiatry in GIMS hospital.
Source of Data: prescription of patients.
Inclusion Criteria:
Exclusion Criteria:
Sample Size: 100 patients will be under taken in this prospective study
RESULTS
TABLE 1. DEPICTING THE AGE WISE DISTRIBUTION OF PATIENTS
|
SR. NO |
AGE GROUP |
NUMBER OF PATIENTS |
PERCENTAGE |
|
01 |
18-30 |
37 |
36.27% |
|
02 |
31-45 |
38 |
37.25% |
|
03 |
46-60 |
22 |
21.56% |
|
04 |
61-75 |
5 |
04.92% |
|
|
TOTAL |
102 |
100% |
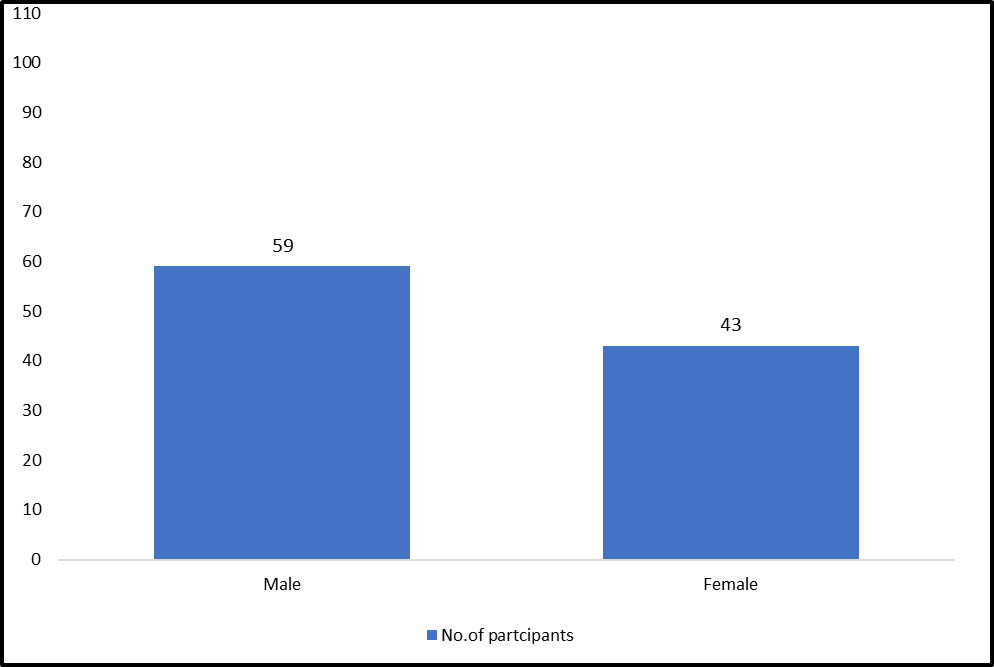
TABLE 2. DEPICTING THE GENDER WISE DISTRIBUTION OF PATIENTS
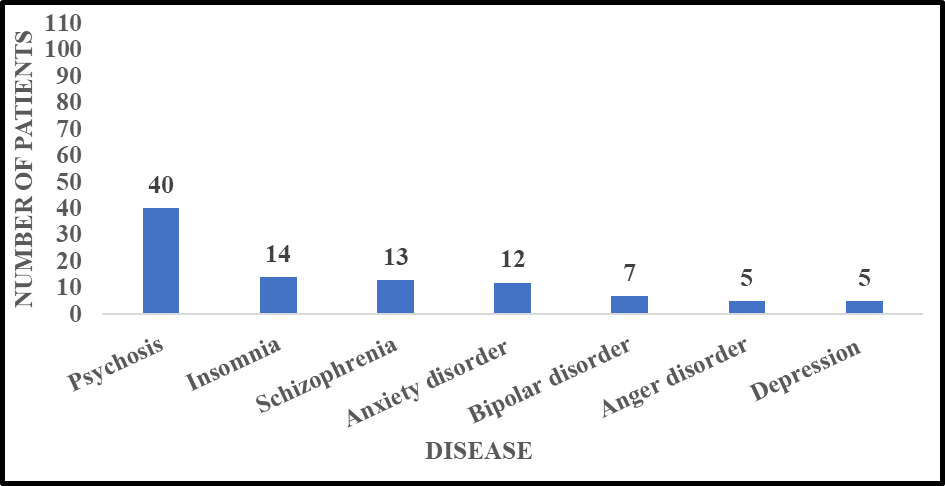
TABLE 3. DEPICTING THE DISEASE WISE DISTRIBUTION OF PATIENTS
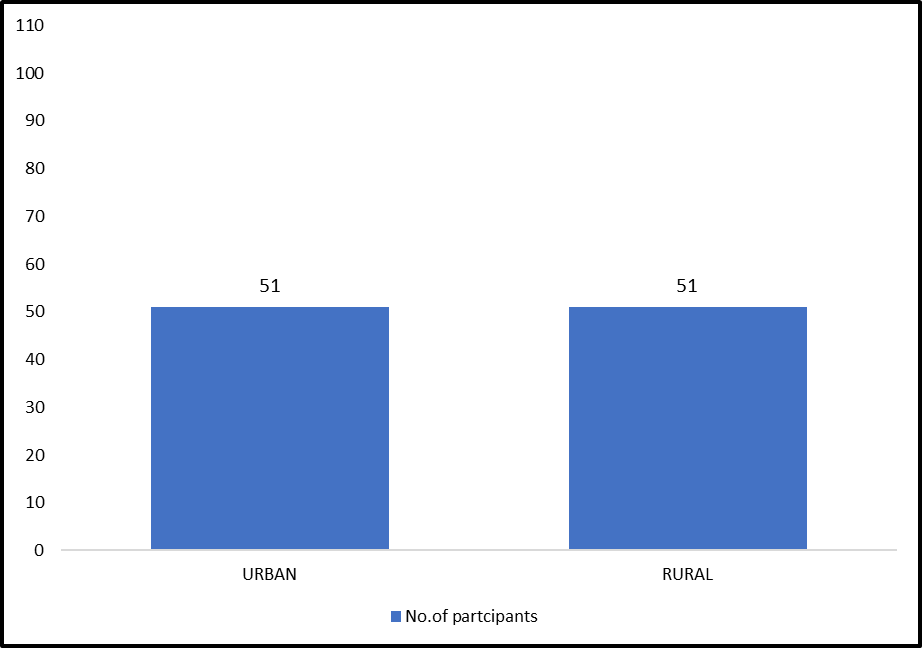
FIGURE4. GRAPH REPRESENTING THE REGION WISE DISTRIBUTION OF PATIENTS
|
SR. NO |
QUESTIONS |
RESPONSE |
|||
|
|
|
PRE |
POST |
||
|
|
|
YES |
NO |
YES |
NO |
|
1 |
Do you sometimes forget to take your Psychotropic medicine? |
93% |
7% |
69% |
31% |
|
2 |
Over the past two weeks, were there any days when you did not take your Psychotropic medicine? |
91% |
9% |
77% |
23% |
|
3 |
Have you ever cut back or stopped taking your medication without telling your doctor, because you felt worse when you took it? |
63% |
37% |
68% |
32% |
|
4 |
When you travel or leave home, do you sometimes forget to bring along your medications? |
50% |
50% |
26% |
74% |
|
5 |
“Did you take your Psychotropic medicine yesterday?” |
84% |
16% |
88% |
12% |
|
6 |
When you feel like your Psychotic symptoms are under control, do you sometimes stop taking your medicine? |
24% |
76% |
31% |
69% |
|
7 |
Taking medication everyday is a real inconvenience for some people. Do you ever feel hassled about sticking to your plan? |
24% |
76% |
18% |
82% |
|
8 |
How often do you have difficulty remembering to take all your Psychotropic medicine |
90% |
10% |
48% |
52% |
DISCUSSION
CONCLUSION
This study concludes that psychiatric disorders were more seen in male patients compared to female patients. Most of the study subjects were from the age group of 31- 45years constituting of 37.25% of total patients. During the study it is observed that Tab RSPN was most commonly prescribed anti-psychotic drug and it was mostly prescribed with Tab THP.
Tab Risperidone, Tab Trihexyphenidyl, Tab Olanzapine, Tab Fluoxetine are most commonly prescribed psychotropic drugs. Most patients were prescribed 2-3 psychotropic medications which included Tab Risperidone, Tab Trihexyphenidyl, Tab Fluoxetine, however polypharmacy must be minimized in psychiatric out patients as it might results in poor compliance, increased drug interactions and side effects. Our study was carried out for a period of 6 months and was mainly confined to Psychiatry Out Patient Department (OPD) in GIMS Hospital. Were we found out that the follow up rate and medication adherence were poor. This study provide baseline for conduct of drug utilization studies periodically for a longer duration over large population size and provide benefits to psychotic patients in near future.
ACKNOWLEDGEMENT
The authors express their gratitude to Dr. ASHOK KUMAR MALPANI, Professor & Principal, RMES’s College of Pharmacy, Kalaburagi for the encouragement and significant support received throughout the research.
AUTHOR’S CONTRIBUTION
All the authors have contributed equally.
CONFLICT OF INTEREST
All authors declare that there are no conflicts of interest.
ETHICS DECLARATION
The Institutional Ethics Committee at RMES’s College of Pharmacy approved the protocol. All residents in the hospital provided informed consent.
CONSENT FOR PUBLICATION
All authors have consented to the publication of their work.
COMPETING INTERESTS
The authors hereby declare that they did not obtain any financial support from any source for the writing or publication of this article
AUTHORS FUNDING
The authors hereby declare that they did not obtain any financial support from any source for the writing or publication of this article.
REFERENCES




Gururaj Wadageri, Shashank Algud, Shivalingayya Mathpathi, Gururaj Mahagaon, Amitkumar Shivgond, Assessment of Prescription Pattern, Follow-Up Pattern and Impact of Pharmacist Initiated Educational Intervention on Medication Adherence in Patients with Psychiatric Disorders, Int. J. of Pharm. Sci., 2026, Vol 4, Issue 1, 384-389. https://doi.org/10.5281/zenodo.18154504
 10.5281/zenodo.18154504
10.5281/zenodo.18154504