
We use cookies to ensure our website works properly and to personalise your experience. Cookies policy

We use cookies to ensure our website works properly and to personalise your experience. Cookies policy
1,2,3,4,5 Rungta Institute of Pharmaceutical Sciences, Kohka, Bhilai, Chhattisgarh-490024, India
6Rungta Institute of Pharmaceutical Sciences & Research, Kohka, Bhilai, Chhattisgarh-490024, India
Moisturizers represent a cornerstone of dermatological therapy, particularly in the management of inflammatory skin diseases. Beyond their fundamental role in hydration, modern moisturizers actively participate in skin barrier repair, reduction of transepidermal water loss (TEWL), lipid matrix organization, and modulation of inflammatory cascades. This comprehensive review examines the structure and function of the skin barrier, the pathophysiology of xerosis, the classification and mechanisms of moisturizer ingredients, their clinical applications across specific dermatoses, safety considerations, formulation science, and future therapeutic directions. Particular emphasis is placed on atopic dermatitis, where moisturizers function as both primary and adjunctive therapy, significantly improving clinical outcomes and patient quality of life. The evolving understanding of the skin as a four-layer functional unit—physical, chemical, microbiological, and immunological—provides a framework for understanding how targeted moisturization strategies can address specific barrier defects.
The skin serves as the body's primary interface with the external environment, performing essential functions that include preventing transepidermal water loss, excluding harmful microorganisms, regulating body temperature, and orchestrating immune responses. In inflammatory dermatoses, this protective barrier becomes compromised, resulting in increased permeability, xerosis, irritation, and susceptibility to secondary infection. Consequently, moisturizers have evolved from cosmetic adjuncts to essential therapeutic tools in dermatology practice.
The term "cosmeceuticals" describes products that bridge the gap between cosmetics and pharmaceuticals, and moisturizers represent one of the earliest and most widely utilized cosmeceutical interventions for maintaining epidermal health and managing cutaneous inflammation. Regular moisturizer use can significantly reduce flare frequency and enhance the efficacy of concurrent pharmacologic therapies. Recent guidelines for the management of atopic dermatitis emphasize the importance of moisturizers as foundational therapy, with recommendations for daily application to both prevent and treat disease manifestations.[1] This review synthesizes current evidence regarding the role of moisturizers in inflammatory skin conditions, with particular attention to their mechanisms of action, clinical applications, safety profiles, and emerging formulation strategies. The goal is to provide a clinically relevant, evidence-based overview suitable for dermatology practitioners, researchers, and trainees.
2. Skin Barrier Structure and Function
2.1 Anatomical and Functional Organization
The epidermis comprises multiple layers, with the stratum corneum serving as the principal barrier structure. Classically described using the "brick and mortar" model, the stratum corneum consists of terminally differentiated corneocytes (the "bricks") embedded within a lipid matrix (the "mortar") composed primarily of ceramides, cholesterol, and free fatty acids. This organization creates a hydrophobic barrier that limits both water loss and external penetrant entry. Contemporary understanding has expanded this model to conceptualize the skin barrier as four interdependent functional layers: physical, chemical, microbiological, and immunological. Each layer contributes uniquely to overall barrier integrity, and disruption of any component can precipitate or perpetuate inflammatory skin disease.[2]
2.2 The Physical Barrier
The physical barrier encompasses the stratum corneum structure, including corneocytes, cornified envelope proteins, and intercellular lipids. Tight junctions between keratinocytes in the granular layer provide an additional paracellular barrier. Filaggrin, a key protein processed into natural moisturizing factors (NMF), maintains hydration and facilitates corneocyte compaction. Mutations in the filaggrin gene (FLG) represent the strongest genetic risk factor for atopic dermatitis, highlighting the physical barrier's centrality in disease pathogenesis.
2.3 The Chemical Barrier
The chemical barrier comprises the "acid mantle" (pH 4.5-5.5), antimicrobial peptides, lipids, and NMF. Optimal acidic pH supports enzymatic function necessary for lipid processing and desquamation while inhibiting pathogenic bacterial growth. NMF, derived from filaggrin breakdown, includes amino acids, pyrrolidone carboxylic acid, and urocanic acid that collectively maintain stratum corneum hydration.
2.4 The Microbiological Barrier
The skin microbiome comprises diverse communities of bacteria, fungi, and viruses that contribute to barrier function through multiple mechanisms. Commensal organisms such as *Staphylococcus epidermidis* produce antimicrobial peptides, compete with pathogens for nutrients and adhesion sites, and modulate local immune responses. This ecosystem maintains homeostasis through complex microbial-host interactions.
2.5 The Immunological Barrier
Keratinocytes, Langerhans cells, and resident T lymphocytes form an immunological surveillance network that recognizes barrier disruption and coordinates appropriate responses. Pattern recognition receptors on keratinocytes detect danger signals and pathogen-associated molecular patterns, initiating cytokine cascades that recruit inflammatory cells when necessary.
2.6 Barrier Disruption in Disease
When any barrier layer is compromised, the skin becomes increasingly permeable to allergens, irritants, and microbes, triggering inflammatory responses that further degrade barrier function. This creates a self-perpetuating cycle central to chronic inflammatory dermatoses. Moisturizers interrupt this cycle by reinforcing barrier structure and function across multiple layers simultaneously.[7]
3. Pathophysiology of Dry Skin (Xerosis)
3.1 Epidemiology
Xerosis describes pathologically dry skin characterized by reduced stratum corneum hydration, rough texture, scaling, and often pruritus. It represents both a standalone condition and a nearly universal feature of inflammatory dermatoses. Population studies demonstrate increasing prevalence with age, affecting up to 75% of elderly individuals.
3.2 Molecular and Structural Alterations
Dry skin results from decreased lipid content, abnormal desquamation, reduced ceramide levels, and impaired keratinocyte differentiation. These changes produce significant elevation in TEWL, the physiologic gold standard for assessing barrier function. In inflammatory skin diseases, FLG mutations and reduced ceramide production exacerbate xerosis and perpetuate inflammation.
3.3 The Itch-Scratch Cycle
Xerosis-induced pruritus triggers scratching behavior that mechanically disrupts the stratum corneum, releasing pro-inflammatory cytokines and further compromising barrier integrity. This itch-scratch cycle represents a critical therapeutic target in conditions like atopic dermatitis, where moisturizer use can interrupt this positive feedback loop.
3.4 Cytokine-Mediated Inflammation
Persistent barrier disruption stimulates keratinocyte release of thymic stromal lymphopoietin (TSLP), IL-25, and IL-33—alarmins that initiate type 2 inflammatory responses. This cytokine milieu promotes further barrier dysfunction, creating a self-sustaining inflammatory state. Moisturizers reduce this inflammatory drive by restoring barrier integrity and limiting alarmin release.[3]
4. Classification of Moisturizer Ingredients
4.1 Occlusives
Occlusives form a hydrophobic layer on the skin surface that physically blocks evaporative water loss. Petrolatum remains the gold standard, reducing TEWL by up to 98% through intercalation into the stratum corneum interstices rather than simply coating the surface. Other occlusives include mineral oil, lanolin, silicones (dimethicone), and various waxes. The selection of occlusive agents requires consideration of cosmetic acceptability, as greasiness may affect patient adherence. Newer formulations incorporate occlusives in ways that balance efficacy with aesthetic properties.
4.2 Humectants
Humectants attract and retain water by virtue of hygroscopic properties, drawing moisture from the dermis and, in humid conditions, the environment into the stratum corneum. Common humectants include:
4.3 Emollients
Emollients fill spaces between desquamating corneocytes, smoothing the skin surface and improving texture. They comprise fatty acids, fatty alcohols, cholesterol, and various esters that intercalate into the lipid bilayer. The term "emollient" is often used interchangeably with "moisturizer" in clinical contexts, though strictly refers to this specific functional category.
4.4 Barrier-Repair Lipids
Modern moisturizers increasingly incorporate physiologic lipids that actively replenish deficient barrier components:
Optimal barrier repair requires specific ratios approximating physiologic composition (approximately 1:1:1 molar ratio of ceramides:cholesterol: free fatty acids). Products formulated with these ratios demonstrate superior barrier repair compared to those containing isolated lipids.
4.5 Anti-Inflammatory Additives
Advanced formulations incorporate ingredients with direct anti-inflammatory properties:
4.6 Formulation Types
The vehicle significantly influences moisturizer function and patient acceptability:
5. Mechanisms of Moisturizer Action
5.1 Reduction of Transepidermal Water Loss
The primary function of occlusive ingredients is to establish a physical barrier that limits evaporative water loss. This reduction in TEWL allows the stratum corneum to rehydrate and supports enzymatic processes necessary for normal desquamation and lipid processing.
5.2 Attraction and Retention of Water
Humectants increase stratum corneum water content through hygroscopic mechanisms. This hydration plasticizes the stratum corneum, improving flexibility and reducing fissuring. Importantly, humectants alone may increase TEWL if used without concomitant occlusives, as enhanced hydration can disrupt lipid organization—emphasizing the importance of combination formulations.
5.3 Lipid Repletion and Barrier Restoration
Exogenous lipids incorporate into the stratum corneum interstices, restoring lamellar bilayer structure. Physiologic lipids additionally stimulate endogenous lipid synthesis through feedback mechanisms. Ceramide-dominant formulations have demonstrated particular efficacy in conditions characterized by ceramide deficiency, such as atopic dermatitis.
5.4 Modulation of Epidermal Differentiation
Moisturizer ingredients influence keratinocyte differentiation and gene expression. Glycerin upregulates filaggrin expression and tight junction proteins. Urea modulates differentiation markers and stabilizes the lipid matrix. These effects extend beyond passive hydration to active modulation of epidermal biology.
5.5 Anti-Inflammatory Effects
Barrier repair reduces antigen penetration and subsequent immune activation, providing indirect anti-inflammatory benefits. Additionally, specific ingredients exert direct anti-inflammatory effects through inhibition of NF-κB signaling, reduced cytokine release, and antioxidant properties. A recent clinical trial demonstrated that moisturizers containing anti-inflammatory ingredients (shea butter, bacterial lysate, allantoin, bisabolol, and botanical extracts) produced significantly greater improvements in skin hydration and SCORAD scores compared to base moisturizer alone.
5.6 Microbiome Modulation
Emerging evidence suggests moisturizers influence cutaneous microbial composition. Emollient use shifts the microbiome toward greater diversity, potentially by improving the physical habitat for commensal organisms. Conversely, excessive occlusion may promote dysbiosis, highlighting the need for balanced approaches.
5.7 Improvement of Biomechanical Properties
Hydration improves skin elasticity and reduces stiffness, decreasing mechanical friction and susceptibility to fissuring. These biomechanical improvements contribute to symptom relief and reduced itch.
5.8 Integrated Multi-Layer Effects
The contemporary four-layer model of skin barrier function provides a framework for understanding how moisturizers simultaneously affect multiple barrier components. Occlusives, humectants, and emollients strengthen the physical barrier. Acidic formulations and urea support the chemical barrier through pH optimization and NMF enhancement. Emollients shift microbiome composition toward greater diversity. Reduced barrier permeability limits allergen penetration and subsequent immunological activation.[7]
6. Clinical Applications in Inflammatory Skin Diseases
6.1 Atopic Derma
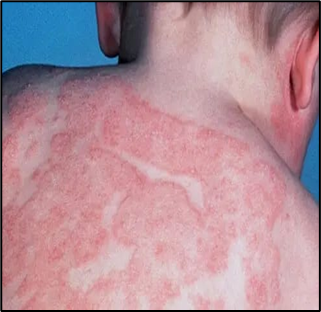
Fig.01 Atopic Derma
Atopic dermatitis (AD) represents the prototypical inflammatory dermatosis where barrier dysfunction drives disease pathogenesis. AD skin demonstrates reduced ceramide levels, FLG mutations in 20-30% of patients, increased serine protease activity, and elevated pH—all contributing to barrier compromise and Th2-polarized inflammation.
6.2 Contact Dermatitis
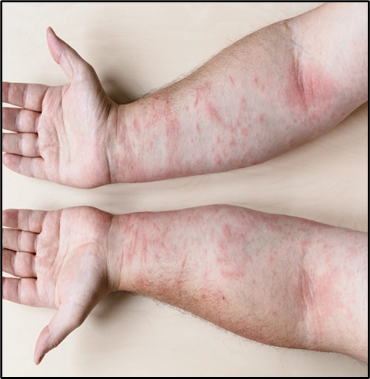
Fig.02 Contact Dermatitis
6.3 Psoriasis
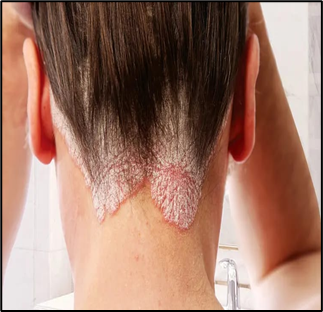
Fig.03 Psoriasis
Psoriasis involves hyperproliferation and abnormal differentiation, with secondary barrier disruption. While moisturizers do not address the primary immune pathogenesis, they provide important symptomatic benefits:
Urea-containing preparations at 10-20% concentrations offer particular benefit through combined humectant and keratolytic effects.
6.4 Acne Vulgaris
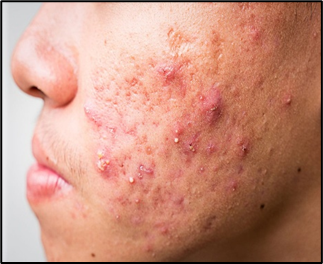
Fig.04 Acne Vulgaris
Moisturizer use in acne requires careful product selection to avoid exacerbation while supporting tolerance of anti-acne therapies. Retinoids, benzoyl peroxide, and topical antibiotics all produce irritant effects that compromise barrier function and reduce treatment adherence.
6.5 Rosacea
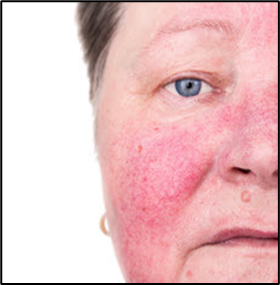
Fig.05 Rosacea
Rosacea skin demonstrates heightened sensitivity and impaired barrier function, particularly the erythematotelangiectatic subtype. Moisturizers reduce irritation, support barrier recovery, and may decrease transepidermal water loss.
Key Considerations: Fragrance-free, minimally formulated products reduce the risk of stinging and irritation. Ingredients with anti-inflammatory properties (niacinamide, azelaic acid, licorice extract) provide additional benefits. Physical sunscreens integrated into moisturizers address photosensitivity, a key trigger factor.
6.6 Other Inflammatory Conditions
7. Special Populations and Regional Considerations
7.1 Pediatric Populations
Infant skin differs structurally from adult skin, with thinner stratum corneum and developing barrier function. Moisturizer selection in this population requires attention to safety and sensitization potential. Recent analysis of top-selling infant skincare products identified frequent inclusion of potential allergens, with preservatives (phenoxyethanol, ethylhexylglycerin, sodium benzoate) and surfactants (cocamidopropyl betaine) most commonly detected. Only 3 of 38 products surveyed contained no identified allergens. These findings emphasize the importance of ingredient scrutiny in pediatric populations.
7.2 Geriatric Populations
Aging skin demonstrates reduced lipid synthesis, decreased sebum production, and diminished NMF content—all contributing to xerosis. Higher lipid content formulations and humectants address these age-related changes. Urea-containing products prove particularly beneficial for elderly patients with pronounced xerosis.
7.3 Asia-Pacific Considerations
Epidemiology and presentation of inflammatory dermatoses vary across regions. In Asia-Pacific populations, atopic dermatitis prevalence remains high, with particular genetic susceptibility factors. Climate variation across the region influences moisturizer selection—higher humidity environments may permit lighter formulations, while arid or air-conditioned environments require more substantial barrier support. Cultural practices and healthcare access significantly influence moisturizer utilization patterns. Regional guidelines increasingly emphasize daily moisturization for flare prevention, though implementation varies across healthcare systems.
7.4 Climate and Environmental Factors
Moisturizer selection should consider environmental conditions:
8. Safety and Adverse Effects
8.1 Irritant Reactions
While generally safe, moisturizers may produce irritant reactions, particularly in already inflamed skin. Potential irritants include:
8.2 Allergic Contact Dermatitis
Moisturizers represent common sources of allergic contact dermatitis due to the wide variety of potential sensitizers they contain:
8.3 Special Safety Considerations
Microbial Contamination: Preservative systems prevent microbial overgrowth; preservative-free products require packaging that prevents contamination.
Systemic Absorption: Minimal for most ingredients, though percutaneous absorption of certain compounds (particularly in compromised skin) warrants consideration.
Occlusion-Related Effects: Excessive occlusion may promote microbial dysbiosis, with theoretical concerns regarding increased S. aureus colonization. A critical review recently questioned whether moisturizers may be overused in dermatitis care, citing potential for microbial dysbiosis with excessive occlusion. This highlights the importance of balanced, evidence-based recommendations.
8.4 Ingredient Selection Guidance
For patients with sensitive skin or contact allergy history, simplified formulations with minimal ingredients reduce sensitization risk. Patch testing can identify specific allergens when contact dermatitis is suspected. Resources such as the American Contact Dermatitis Society's Core Allergen Series guide ingredient avoidance based on patch test results.[7]
9. Patient Education and Treatment Adherence
9.1 The Adherence Challenge
Despite strong evidence supporting moisturizer efficacy, adherence remains suboptimal. Common barriers include:
9.2 Practical Application Instructions
Effective patient education includes specific guidance:
9.3 Product Selection Guidance
Help patients navigate product selection by considering:
9.4 Educational Strategies
Structured educational programs improve outcomes:
9.5 Measuring Adherence and Outcomes
Objective measures (TEWL, corneometry) provide feedback on barrier status. Patient-reported outcomes (itch scores, DLQI, POEM) capture subjective improvement. Regular follow-up supports continued adherence and allows formulation adjustment.[1]
10. Future Perspectives and Advanced Formulations
10.1 Microbiome-Supportive Skincare
Recognition of the skin microbiome's role in barrier function has spurred development of microbiome-targeted formulations:
The global microbiome skincare market is projected to reach $1.44 billion by 2034, driven by consumer demand for personalized, barrier-supporting formulations.
10.2 Nanotechnology and Delivery Systems
Advanced delivery systems enhance ingredient penetration and targeting:
10.3 Personalized and Precision Approaches
The future of moisturizer therapy likely involves personalization based on individual characteristics:
-Genetic profiling FLG mutation status may guide ceramide or NMF supplementation
- Lipid profiling: Individual ceramide composition could inform targeted repletion
- Microbiome analysis: Personalized probiotic/prebiotic formulations based on individual dysbiosis patterns
- Biomarker-guided therapy: Inflammatory markers may guide anti-inflammatory additive selection
10.4 "Emollients Plus" and Combination Products
Formulations combining barrier repair with active therapeutic ingredients represent an evolving category:
A recent 12-week trial of herbal emollients containing ginger extract and cannabidiol demonstrated progressive improvement in AD outcomes with excellent tolerability, supporting the "emollients plus" concept.
10.5 Biomimetic Formulations
Increasing sophistication in replicating natural skin composition:
10.6 Sustainability Considerations
Environmental concerns increasingly influence formulation and packaging:
11. Critical Appraisal and Research Gaps
11.1 Limitations of Current Evidence
Despite widespread use, significant evidence gaps remain:
11.2 Methodological Considerations
Future research should address:
CONCLUSION
Moisturizers have evolved from simple cosmetic preparations to sophisticated therapeutic agents that actively participate in skin barrier repair, inflammation modulation, and disease prevention. Understanding the skin as a four-layer functional unit—physical, chemical, microbiological, and immunological—provides a framework for appreciating how moisturizers exert their multifaceted effects. In atopic dermatitis and other inflammatory dermatoses, moisturizers serve as foundational therapy, reducing flare frequency, decreasing pharmacologic requirements, and improving quality of life. The evidence supporting regular moisturizer use is robust, though significant questions remain regarding optimal formulation selection, frequency, and long-term outcomes. Clinical success requires appropriate product selection matched to individual patient characteristics, thorough education regarding proper application technique, and ongoing support to maintain adherence. Future developments in microbiome-targeted formulations, personalized approaches, and advanced delivery systems promise to further enhance the therapeutic potential of these essential dermatologic tools.
The integration of moisturizers into comprehensive management strategies—combining barrier repair with anti-inflammatory therapy, patient education, and multidisciplinary care—offers the greatest potential for improving outcomes in patients with inflammatory skin conditions. As research continues to elucidate the complex interactions between barrier function, inflammation, and microbial ecology, moisturizer formulations will undoubtedly become increasingly sophisticated and targeted, fulfilling their promise as true therapeutic agents rather than simple cosmetic adjuncts.
REFERENCES






Anshika Singh Chauhan, Bharti Rao, Prerna Bahekar, Rony Saha, Dewanjali Rathore, Dr. Gyanesh Kumar Sahu, The Role of Moisturizers in Inflammatory Skin Conditions: A Comprehensive Review, Int. J. of Pharm. Sci., 2026, Vol 4, Issue 2, 4505--4517. https://doi.org/10.5281/zenodo.18799990
 10.5281/zenodo.18799990
10.5281/zenodo.18799990